Health
What does circumcision healing look like?
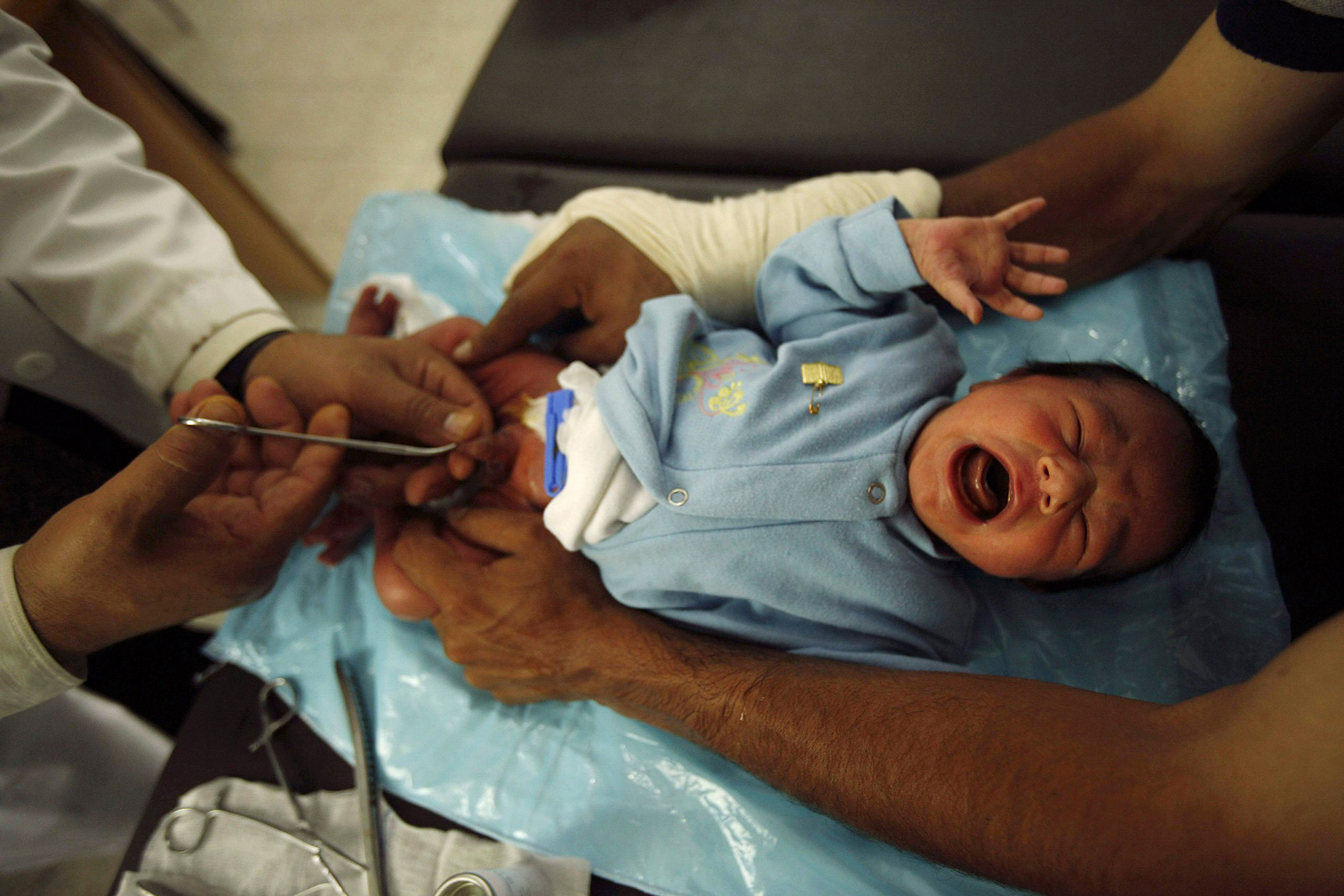
What does circumcision healing look like?
Newborn boys have a piece of skin at the head of their penis called the foreskin. Circumcision refers to a surgical process in which the foreskin is removed. A baby’s circumcision is often performed during the first 7 to 10 days following birth. It will happen in a hospital at home by professional doctors or surgeons.
Your pediatrician or family physician will do the procedure before you bring your child home if you wish to have your boy circumcised. The doctor can explain the procedure to you as well as any potential dangers.
If the circumcision is performed after the first 10 days, it may be more complex and include the use of general anesthesia to put the baby to sleep and lessen the pain. You must consult professional and expert doctors to get your baby circumcised. Learn more to know about the best doctors who perform circumcision in the safest way by using advanced techniques.
Circumcision Healing Process
You will most likely witness a white to yellow to grey “wet scab” when the circumcision heals rather than a red “bloody” one. This is not pus; it is just the usual healing process. Avoid accidentally wiping it off because doing so will delay the penis’s recovery time.
Your child’s penis can appear red and swollen after circumcision. The doctor may have performed the circumcision using a Plastibell ring. If so, your child’s penis will be wrapped in a piece of plastic. In 10 to 12 days, the ring will come off naturally.
The day following the treatment, a thin, yellow coating could develop over the area. This indicates that a circumcised penis has started to heal. While the area heals, your infant can be irritated or may experience pain when urinating. However, the pain and redness usually go away after three to four days of the process.
In some cases. The healing can takes two to three weeks. The main aspects of routine circumcision healing include:
-
Slightly red and tender for 2 to 3 days
-
A plastibell ring should fall off naturally after 10 to 14 days
-
In 7 to 10 days, the scab along the incision line falls off.
Circumcision Aftercare
DO use any brand of diaper wipes or soap and water to keep the penis and diaper as clean as you usually would. If the umbilical cord is still intact, sponge bathing is advised for bathing. If it has been more than 24 hours since the circumcision, a submerged bath is acceptable if the cord has already been cut and dried.
Keep lubricating the tip of the penis with petroleum jelly or A & D ointment. Put a dab of petroleum jelly on the penis or the front of the nappy for 3 to 5 days, even after the dressing is no longer required. Your infant may experience less discomfort as a result of rubbing and nappy sticking.
Petroleum jelly can be used directly on the penis or sterile or non-sterile gauze. The gauze keeps the ointment on the penis’ tip and keeps feces away from it. Do not worry about the little things because it is challenging to keep this area clean, and he will urinate and poop all over it soon enough. It is quite uncommon for the tip to become infected following circumcision.
The average time it takes for a penis to heal is usually between 7 and 10 days. At first, the penis tip could seem a little swollen and red, and there might be a little blood on the diaper. After a few days, you could also detect a faintly yellow discharge or crust, indicating a recovery.
When to See a Doctor?
Circumcision is a safe process that heals naturally within 7 to 10 days. However, you must take care of the circumcised penis at home according to the instructions of the doctor. However, if you see the following signs in your child after circumcision, you must seek urgent medical assistance.
-
Your baby is suffering from a high fever
-
Your baby is feeling irritated or fussy
-
Baby does not urinate even after 12 hours of circumcision
-
Bleeding more than usual
-
If the circumcised area is getting infected, such as redness, swelling, or a red streak
Health
8 shocking health benefits of selenium

Table of Contents
Health
15 shocking health benefits of coriander leaves

Table of Contents
Discover the 15 shocking health benefits of coriander leaves
There are many health benefits of coriander leaves that you can get which are very helpful as disease prevention and natural treatment method.
Besides, it is very easy to consume these coriander leaves, since you can combine them with other spices when you prepare your food.
Here are several health benefits of coriander leaves that you can get by consuming them in your diet.
1.- Antibiotic
The first health benefits of coriander leaves that you can get are for the antibiotic effect.
Especially when it is used as a treatment for digestive problems, for example, diarrhea that causes pathogens, so they need some antibiotics to cure it.
The reason is that within this plant there are borneol chemicals that can treat various health symptoms such as measles, gastric inflammation, hemorrhoids, flu, vertigo, high blood pressure, vomiting, breast inflammation, and even impotence.
2.- Antioxidant
Many studies are done to show the effectiveness of coriander leaves as an antioxidant.
Among the benefits of coriander leaves, there are antioxidant substances such as chlorogenic acid and caffeic acid, capable of fighting free radicals that cause skin oxidation.
Therefore, if you consume these coriander leaves as part of your daily intake, you will be able to protect your skin from wrinkles due to that free radical.
It turns out that the health benefits of coriander leaves are also usable for cancer.
Especially since there are many types of antioxidants within these leaves that can prevent cancer, such as Vit E, Vit C, caffeic acid, beta carotene, ferulic, kaempferol, and quercetin.
These substances are especially effective in reducing oxidative stress that can cause cancer.
Therefore, if you want to reduce your chances of developing cancer, then you may want to consume coriander leaves regularly.
4.- Inflammation
Among the benefits of coriander leaves, there is one of the most important essential oils is cineole.
Also, within these leaves, there is a component of linoleate acid.
Those two substances are great, especially for protecting you from various problems, like rheumatism and arthritis.
This is also suitable to be used as a treatment for inflammation, especially that which occurs on the skin.
Within these leaves is also atsiri oil, which is especially useful when used against infections caused by bacteria and fungi.
Because there is a lot of substance available within the leaves, it can be used as an antifungal, antiseptic, and disinfectant.
The antioxidant within these leaves is very powerful, so you can even use it to treat eczema and other skin problems.
5.- Heart
The health benefits of coriander leaves are also helpful for those experiencing any problems with their heart condition.
For those who have hypertension, try to consume this because it can lower your blood pressure effectively.
Especially since the calcium and cholinergic ion within these leaves are exceptionally effective in reducing the risk of developing cardiovascular disease, which also includes heart attack and stroke.
The essential oil within these leaves will also make your heart work better.
6.- Diarrhea
Inside the leaves are several essential oils that can make your digestion system work better, such as linalool and borneol. They can make your stomach work better.
Furthermore, you can even use the leaves to cure various digestion system problems such as diarrhea.
The reason is that within the leaves is a helpful substance that can treat diarrhea symptoms such as beta phellandrene, cineole, limonene, borneol, and alpha-pinene.
These substances are known for their antibacterial properties so they can cure the symptoms of diarrhea.
You can also consume coriander leaves when you want to vomit or nausea to relieve symptoms.
7.- Cholesterol
Cholesterol is very bad, as it can cause many types of diseases when not properly treated, such as a heart attack, diabetes, stroke, and many others.
So, if you want to lower the level of available cholesterol in your blood, try consuming these coriander leaves.
The leaves that contain potassium and sodium will be able to reduce them effectively as one of the health benefits of coriander leaves.
Other types of acidic substances that are known to effectively lower the level of available cholesterol within your blood are also available within these leaves, such as linoleate acid, palmitate acid, oleate acid, askorbat acid, as well as stearate acid.
Those substances within the leaves can reduce cholesterol buildup within the vein and artery wall. What’s more,
8.- Iron
These coriander leaves are also known as a good source of iron which is very helpful for many kinds of functions in your body.
First, it is used to make your bone healthy. It is also important in the formation of hemoglobin within your blood, as it will be used to carry oxygen throughout the body.
That is why; If you lack this iron nutrient, your heart beats too fast, you will feel great fatigue and various problems in your respiratory system.
It is also an important nutrient that can prevent anemia from happening to you.
9.- Eyes
As you know, the health benefits of coriander leaves are also very useful for your eyes.
Especially because within these leaves there is a beta carotene substance which is a form of Vit A.
Vitamin A is necessary for your eyes to become healthier and maintain their condition.
Additionally, the antioxidant within the leaves can prevent various eye problems such as cataracts and even macular degeneration.
Health benefits of coriander leaves
10.- Mouth ulcer
Within the leaves, you can also find citronellol, which is a very effective antiseptic.
That is why; you can use it effectively to treat mouth ulcers as it can make the healing process faster and also make your breath feel fresh afterward.
That could be why you may find coriander leaves used as an ingredient in toothpaste.
In the old days, when there was no toothpaste, the leaves were used to eliminate bad breath.
11.- Detoxification
Detoxification is a very important thing because the heavy metal inside your body can cause many kinds of problems in the future, such as autism, dementia, and infertility.
But don’t worry, as the health benefits of coriander leaves can also be used for the detox process.
These sheets are exceptionally effective when used to remove heavy metals that are very dangerous to your body, such as aluminum and even mercury.
12.- Insomnia
There is a time when you can’t sleep even though you don’t really think about anything and aren’t even stressed during the day.
Even though your body is already tired, sometimes you still have trouble sleeping properly.
The reason could be because the chemical composition within your body is an imbalance that makes your body unable to function properly.
This will stiffen your nerves so you will have trouble falling asleep.
When that happens, you may want to try the consumption of coriander leaves, as inside you can find phytonutrients and other substances capable of balancing the chemical composition of the body.
After the chemical composition within your body balances, your nerves will relax and you can easily fall asleep.
13.- Urolithiasis
Other health benefits of coriander leave that you can get come from the natural diuretic properties that this leaf has.
Due to these properties, the consumption of these coriander leaves will be able to promote urine production.
Hence, this sheet is also very effective when used to prevent urolithiasis from occurring.
Also, these leaves that have detoxification properties will detoxify your kidney.
This may reduce the risk of developing kidney stones in the future.
That is why; it is very good for you to consume this coriander regularly.
14.- Diabetes
You should know that by consuming coriander leaves, you will be able to activate your endocrine gland to work.
Furthermore, it will also cause the pancreas to produce more insulin, thereby increasing the level of insulin within the blood.
This insulin will be able to effectively dissolve the sugar in the blood, thus lowering the blood sugar level.
This is an exceptionally important process, especially for you, who have diabetes, so your blood sugar level will decrease by consuming these leaves.
Also, even when you do not have diabetes, consuming coriander leaves may reduce your risk of diabetes.
It can also make your body metabolize sugar better.
Therefore, it is still good for everyone to consume these coriander leaves regularly
15.- Vitamin K
You should know that within these leaves, you can also find vitamin K which has many health benefits from coriander leaves.
If you lack this nutrient, then your body will not be able to process blood clotting because the blood thickening process will be favored with the use of this vitamin K.
Therefore, if you do not get enough vitamin K within your body, then you will keep bleeding every time you get hurt, which will be very dangerous for your life.
Those are several health benefits of coriander leaves that you can get and are exceptionally helpful for treating and even preventing various diseases.
Within these leaves are a large number of essential oils that you can find that also have several useful properties for your health.
You can use these leaves as a natural treatment for various symptoms because the properties these leaves contain are very powerful in treating various diseases.
But it is not only useful as a treatment, this is also useful as prevention of those diseases in the first place.
That is why; The best thing for you is that you can consume these leaves regularly as it is often used as food.
But you should know that some of you might develop allergies after consuming these leaves.
Especially those who often experience allergies to spices so you need to know if you have an allergy when consuming coriander leaves or not.
If you have an allergy, you will also experience irritation to your skin.
So, try taking a little to see the effect before consuming it directly.
Health
16 Benefits of Taurine and side effects

Discover the 16 Benefits of Taurine and side effects.
Taurine is a semi-essential organic compound. Although scientists have known it for more than two centuries; The health benefits of taurine have recently become clear.
A diet rich in taurine can protect the body and promote longevity.
Taurine supplements are non-toxic, cheap, and freely available. Read on to understand why you should consider taurine supplementation and not believe its bad reputation.
Benefits of Taurine
Taurine supplements are recommended for some people, depending on their specific health goals and medical conditions, but it’s important to understand the details of dosage and potential effects.
The most impressive taurine benefits include the following:
•Treatment of Parkinson’s disease
•Improving athletic performance
•Preventing heart disease
•Reducing the risk of diabetes
•Weightloss
•Preventing metabolic syndrome
•Reduce periodontal disease
•Improving muscle growth
1.- Antioxidants
Tissues exposed to oxidative damage have particularly high concentrations of taurine. Like other antioxidants, taurine benefits by directly and indirectly removing harmful oxidants to minimize tissue damage.
Through its antioxidant and anti-inflammatory activities, taurine can protect our bodies from unnecessary cell death and tissue damage.
2.- Reduce inflammation
The antioxidant action of taurine benefits produces taurine chloramine (Taul) and bromine (TauBr), which also have anti-inflammatory properties.
Taurine supplementation enhances the formation of TauCl and TauBr in the body and may be effective in treating inflammatory conditions.
Taurine is very effective in treating acute inflammation (caused by infection, irritants, damaged cells, or cancer). However, its role in the progression of inflammatory diseases (such as arthritis) is less clear.
Decreased Taul generation in the body can worsen inflammation-related joint damage in rheumatoid arthritis.
Taul injections improved arthritis symptoms in various experimental animal models.
The gene for the taurine transporter (TauT) has also been linked to the inflammatory response.
3.- Fight infections
The antimicrobial effects of taurine benefits in the body come from taurine chloramine (Taul) and taurine bromine (TauBr) formation.
Taul and TauBr are capable of killing a wide spectrum of bacteria, fungi (yeasts and molds), viruses, and parasites.
Both Taul and TauBr are promising treatments for infections such as chronic sinusitis, otitis media (swimmer’s ear), acne vulgaris, and gum disease.
Taul and TauBr break down quickly in our bodies and are only effective if used topically, not supplemented. However, taurine supplementation can increase the production of these compounds in our bodies.
Taurine’s role as an antioxidant is also important for the protection of the cells of our immune system.
Taurolidine, another taurine derivative, is commonly used in Europe and the US to help treat various infections.
The white blood cells (neutrophils) of rats supplemented with taurine have an increased ability to destroy invading bacteria.
4.-Help fight cancer
Taurolidine, a taurine derivative that is converted to taurine within the body, increased cancer survival rates in animal models; it also blocked the growth of colorectal cancer in rats.
Cancer patients have reduced levels of taurine. Surgery and chemotherapy further lower taurine levels and can reduce taurine in cancer patients. Therefore, taurine supplementation can be very beneficial for cancer patients.
5.-Treat diabetes
Antioxidants, such as taurine, are low in diabetic individuals. This increases the risk of oxidative damage; diabetes decreases the body’s ability to absorb taurine.
Diabetic complications, such as heart, kidney, and nerve damage, can be attributed to high oxidative damage as a result of low taurine levels.
In a study of 39 types 1 diabetic patient, oral supplementation with 500 mg of taurine three times daily for 3 months restored blood taurine levels. Taurine supplementation also prevented blood cells from clotting, lowering the risk of a heart attack.
In rats, taurine also lowers blood glucose by interacting with insulin receptors on cells.
The role of taurine benefits in protecting the kidneys from damage in diabetes is well documented in animal models and human cells.
One and a half grams of taurine daily for two weeks improved early cardiac abnormalities in a study (DB-RCT) of nine types of diabetic patients.
6.-Protects the heart
Cells of the heart and blood vessels contain the taurine transporter, suggesting that the benefits of taurine are important for heart function.
Heart disease induced by taurine-deficient diet in various animal studies.
The risk of chronic heart disease is lower in individuals with a high urinary production of taurine.
In a study of 22 healthy middle-aged women, 3 g of taurine supplements daily for 4 weeks lowered homocysteine levels. Since homocysteine correlates with heart disease, taurine may help prevent heart attacks or high cholesterol.
Taurine can also prevent abnormal heartbeats (AFib)
Taurine supplementation is effective in treating the hardening and narrowing of blood arteries in animals.
Although more research is needed, the positive effects of taurine’s benefits on the heart are thought to:
•Improves fat profile
•Helps control calcium ion uptake and thus cell excitation
•Acts as an antioxidant
•Prevents contraction of blood vessels
7.- Prevents hypertension
Taurine can increase the production of endorphins by the brain (hypothalamus). This calms the brain’s fight or flight response, which is overactive during stress, and lowers blood pressure.
Low levels of taurine are associated with increased blood pressure.
Oral taurine supplementation is potentially a very safe and convenient regimen for the control of high blood pressure.
Consumption of 3g of taurine per day for 2 months in hypertensive patients reduced both systolic and diastolic blood pressure.
It also plays a protective role in the heart and kidneys in rats with hypertension.
8.- Reduces cholesterol
Taurine supplementation can improve bile secretion and activity and improve the body’s breakdown of cholesterol.
It is also essential for the formation of bile salts and as such plays an important role in the absorption and breakdown of fats and cholesterol.
Additionally, taurine can lower blood and liver cholesterol levels in animals fed a high-fat diet.
9.-Protects the liver
Taurine supplementation in the diet at doses greater than 500 mg daily for 3 months reduced liver injury in 24 patients with chronic hepatitis.
In rats, dietary taurine protected their livers from damage related to heavy metals and oxidized fat.
Taurine availability in the body is low in various forms of liver cirrhosis. In 35 patients with liver cirrhosis, daily taurine supplementation increased taurine levels and also reduced painful muscle cramps that are associated with cirrhosis.
In animal models, taurine is effective in preventing non-alcoholic fatty liver disease. It reduced oxidative stress, cell death, and fat accumulation in the liver.
Taurine supplementation also prevented alcoholic fatty liver disease in animals by decreasing alcohol-induced oxidative stress and inflammation. It also increased the production of proteins associated with the breakdown of fats in the liver.
Animal studies suggest that taurine prevents long-term liver damage and helps liver cells recover more quickly from fatty and alcoholic liver disease.
10.- Parkinson’s disease
Research has shown that when people have adequate or high levels of taurine in their system, neuronal cell regrowth is possible, which may help reverse or mitigate the effects of certain neurodegenerative diseases, such as Parkinson’s disease.
11.- Weight loss
Lowering fat levels in the bloodstream and helping the body deal with excess blood glucose are two of the best benefits of taurine; therefore, they can help optimize the process of weight loss and fat burning.
12.- Athletic performance
This organic compound has become a very popular training supplement as it is known to allow muscles to work longer, safer, and more efficiently, which means your workouts will have better results and your recovery time will be faster. shorter.
13.- Immune function
Having adequate levels of taurine in your body can help your immune system regulate its actions, meaning your body is less likely to experience allergic reactions and other unnecessary energy expenditure.
14.- Muscle development
Taurine benefits are known to aid in skeletal muscle differentiation, and later in life, having adequate levels can help you grow and strengthen your muscles more effectively, making it a popular additive for bodybuilders and powerlifters. dumbbells.
15.- Protects vision
Taurine benefits protect retinal cells from damage caused by oxidants and bright light; In a study (DB-CT) of 62 patients, a combination of taurine, diltiazem, and vitamin E helped decrease vision loss by protecting against oxidative damage.
Low levels of taurine are associated with cataract formation in humans.
In cats, taurine deprivation causes vision loss.
In rats, the antiepileptic drug Vigabatrin depletes retinal taurine. As a result, prolonged use of this drug can lead to irreversible vision loss.
16.- It is good for lung health
The antioxidant activity benefits of taurine can protect the lungs from damage caused by exposure to toxins such as cigarette smoke.
Taurine-fed hamsters can resist lung damage caused by exposure to air pollutants.
Maintenance of tissue taurine levels is critical for the prevention of oxidant-induced lung injury in rats.
In sheep, the taurine-derived taurolidine (which is converted to taurine in the body) prevents lung damage caused by bacterial toxins.
Frequently asked questions about the benefits of taurine
-What is taurine?
Taurine (L-taurine or 2-aminoethane sulfonic acid) is a sulfur-containing amino acid.
Mammals have taurine in almost all tissues, but the heart, brain, retina, platelets, and glands contain particularly high amounts.
Taurine plays a crucial role in the development and protection of cells within mammals; controls multiple important biological processes in the body.
In this sense, taurine could be more easily compared to sodium or calcium ions than to a drug that targets a specific receptor in our body.
Humans are capable of producing taurine, but not in sufficient quantities. Therefore, taurine is a conditionally essential amino acid for humans; Some conditions in which patients may be deficient in taurine include premature infants, newborns, and patients with chronic liver, heart, and kidney disease.
This supplement is also an osmolyte. This means that it controls the entry and exit of water in the cells and prevents them from changing the cell too much; It interacts with fats in cell membranes and stabilizes them, preventing structural changes in the cell.
Despite the impressive range of positive effects that taurine has on the body, its exact mechanisms of action remain largely unknown.
-How does the body produce taurine?
Taurine is synthesized in the body from the only other two sulfur-containing amino acids, methionine and cysteine.
Taurine synthesis occurs primarily in the liver, with the help of the enzyme cysteine sulfinic acid and vitamin B6 (pyridoxine).
Other cells in our body can absorb taurine from the blood thanks to the special taurine transporter molecule (TauT) found in cell membranes.
Taurine is an essential nutrient for newborns as they are not yet able to synthesize or retain taurine within their bodies. Breast milk contains the full taurine requirement for infants, as does modern infant formula.
-How does the body eliminate taurine?
Taurine leaves the body as part of the bile or urine.
The kidneys can increase or decrease taurine excretion depending on the dietary availability of taurine. High amounts of taurine in urine indicate high dietary intake.
Taurine carrier molecules in the kidneys use energy to reabsorb and retain taurine in the body.
People with compromised kidney function or defective taurine transporters may not be able to retain sufficient amounts of taurine.
Taurine Side Effects
Taurine remains one of the most important organic compounds within the body, but there are some potential side effects when consuming too much, such as pregnancy complications and worsening of certain nervous system disorders.
Bipolar Disorder: Studies have found that regular or prolonged use of this compound can worsen the symptoms of bipolar disorder, although, in moderate amounts, it may have a mitigating effect on this condition.
Pregnancy: Some of the more popular taurine supplements also contain other active ingredients, including caffeine, that may pose a risk to pregnant or lactating women, so these individuals should avoid the use of this non-essential amino acid.
Dosage
Up to 3 g of supplemental taurine per day is safe for consumption in adults. There is strong evidence that there are no side effects at doses up to and below this value. Scientists do not recommend a dose greater than 3 g per day.
Relatively high amounts of taurine are safe for consumption because any excess can be passed harmlessly through urine.
-

 Food8 months ago
Food8 months ago10 + Benefits of carrot juice and side effects
-

 Food8 months ago
Food8 months ago8 shocking benefits of leek juice and side effects
-

 Health8 months ago
Health8 months agoBenefits of guava leaves Sensually
-

 Health8 months ago
Health8 months ago5 Shocking health benefits of kinkeliba and side effects
-

 Health8 months ago
Health8 months ago7 health benefits of cashew leaves and side effects
-

 Health8 months ago
Health8 months ago13 shocking health benefits of Thai eggplant
-

 Health8 months ago
Health8 months ago10 shocking health benefits of Canary seed milk
-

 Food6 months ago
Food6 months ago19 Benefits of tobacco plant and side effects
